Management of Peripheral Artery Disease (PAD)
- Home
- Management of Peripheral Artery Disease (PAD)
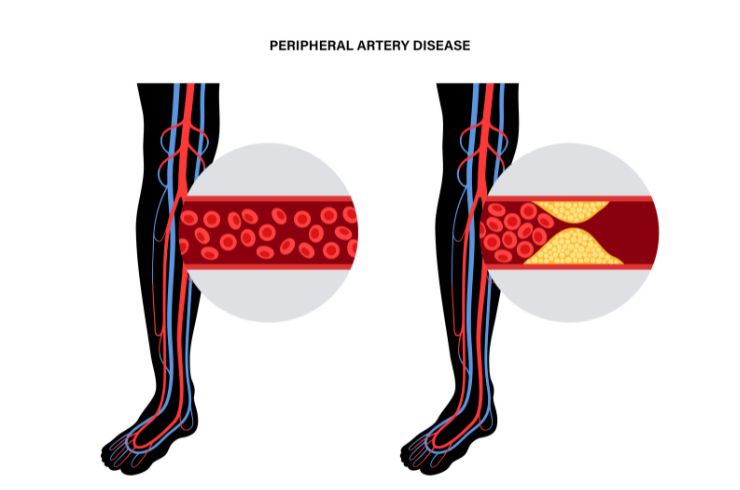
Peripheral Artery Disease (PAD) is a condition in which the arteries supplying blood to the limbs, particularly the legs, become narrowed or blocked due to atherosclerosis (plaque buildup). This reduces blood flow, causing symptoms such as leg pain, cramping, and in severe cases, non-healing wounds or even limb loss. Proper management of PAD focuses on improving blood flow, relieving symptoms, and preventing complications.
Goals of PAD Management:
- Improve blood flow to the affected limbs.
- Relieve symptoms, particularly leg pain and cramping.
- Prevent further complications such as heart attack, stroke, and limb amputation.
- Improve overall quality of life.
Lifestyle Modifications:
- Smoking Cessation:
- Why: Smoking is a major risk factor for PAD, as it accelerates the process of atherosclerosis and worsens blood vessel health.
- Action: Quitting smoking is the most important lifestyle change for PAD patients. It improves circulation and reduces the progression of the disease.
- Exercise:
- Why: Regular exercise improves circulation, increases walking distance, and reduces symptoms like claudication (leg pain during walking).
- Action: A supervised walking program is often recommended. Patients should aim for at least 30 minutes of moderate-intensity exercise, such as walking, most days of the week.
- Healthy Diet:
- Why: A heart-healthy diet helps manage cholesterol levels, blood pressure, and weight, all of which can improve PAD symptoms.
- Action: Adopt a diet low in saturated fats, refined sugars, and processed foods, while increasing the intake of fruits, vegetables, whole grains, and lean proteins.
- Weight Management:
- Why: Maintaining a healthy weight can improve overall vascular health and reduce strain on the circulatory system.
- Action: Weight loss, particularly for overweight or obese individuals, can improve symptoms and overall health.
Medications:
- Antiplatelet Agents:
- Why: Medications like aspirin or clopidogrel (Plavix) are used to prevent blood clots, which can worsen PAD by blocking blood flow to the limbs.
- Action: Antiplatelet therapy reduces the risk of heart attack, stroke, and further complications from PAD.
- Statins:
- Why: Statins lower cholesterol levels and help prevent the progression of atherosclerosis in the arteries.
- Action: Statins, such as atorvastatin or rosuvastatin, are prescribed to reduce the risk of cardiovascular events and improve vascular health.
- Blood Pressure Medications:
- Why: High blood pressure can worsen PAD by further damaging blood vessels.
- Action: Medications like ACE inhibitors, angiotensin receptor blockers, or calcium channel blockers may be used to control blood pressure and improve blood flow.
- Cilostazol:
- Why: Cilostazol is a medication that can improve walking distance and relieve claudication (pain during walking) by improving blood flow.
- Action: It’s particularly useful for symptomatic relief in PAD patients with intermittent claudication.
Endovascular and Surgical Interventions:
- Angioplasty and Stenting:
- Why: In some cases, PAD may be treated with angioplasty, where a balloon is inflated to open up narrowed arteries. A stent (a small mesh tube) may be placed to keep the artery open.
- Action: This procedure restores blood flow to the affected areas, reducing symptoms like pain and improving mobility.
- Bypass Surgery:
- Why: When angioplasty or stenting is not feasible, bypass surgery may be performed to create a new route for blood to flow around the blockage.
- Action: A bypass graft is used to reroute blood flow around the blocked area of the artery, improving circulation to the legs.
- Endarterectomy:
- Why: This procedure involves the surgical removal of plaque from the artery to restore normal blood flow.
- Action: It is used in cases where the artery is blocked but can be cleaned surgically.
- Amputation (in severe cases):
- Why: In very severe cases where PAD leads to tissue death or gangrene, amputation may be necessary to prevent infection and save the patient’s life.
- Action: Amputation is generally a last resort when all other treatment options fail to restore blood flow or heal non-healing wounds.
Monitoring and Follow-up:
- Regular Check-ups: Patients with PAD should have regular follow-up appointments to monitor their symptoms, assess the effectiveness of treatments, and make necessary adjustments.
- Wound Care: For patients with open sores or ulcers due to PAD, wound care is essential to prevent infection and promote healing.
- Vascular Studies: Tests such as ankle-brachial index (ABI), ultrasound, or CT angiography may be used to monitor the progress of PAD and the success of treatments.
Preventing Complications:
- Control underlying conditions: Managing diabetes, high blood pressure, and high cholesterol can prevent further damage to the arteries and improve PAD outcomes.
- Educate patients: Encouraging patients to avoid prolonged sitting or standing, wearing compression stockings, and elevating the legs can reduce swelling and promote better circulation.
Interventions Offered
- Ultrasound-Guided FNAC/Biopsy
- Percutaneous Drainage Procedures
- Soft Tissue & Joint Injections (PRP)
- Spinal Infiltrations
- Nerve Blocks for Pain Management
- Trans Arterial Micro Embolization (TAME)
- PTBD & Biliary Stenting
- PCN & Ureteral Stenting
- Bronchial Artery Embolization for Hemoptysis
- Prostatic Artery Embolization for BPH
- Uterine Artery Embolization for Fibroids
- Varicocele Embolization
- Genicular Artery Embolization for Knee Osteoarthritis
- TACE / TARE for Liver Cancer Treatment
- Thyroid Nodule & Tumor Ablation
- Transjugular Intrahepatic Portosystemic Shunt (TIPS)
- EVLA (Endovenous Laser Ablation) & Sclerotherapy for Varicose Veins
- Thromboaspiration & Catheter-Directed Thrombolysis (CDT) for DVT & Pulmonary Thromboembolism
- Management of Peripheral Artery Disease (PAD)